Would you like to continue or select additional body parts?
- Home
- Treatments
- Surgical
Percutaneous Discectomy Surgery
Normally, the discs in between the bones (vertebrae) of your spine don’t cause you any problems. And even if they do flare up, it’s often possible to manage disc injuries conservatively with treatment such as physical therapy. However, if you develop a condition such as a herniated disc and the pain doesn’t improve in time, you might benefit from a procedure known as a percutaneous discectomy.
WHAT IS A PERCUTANEOUS DISCECTOMY?
A percutaneous discectomy is a minimally invasive procedure used to treat damaged spinal discs.
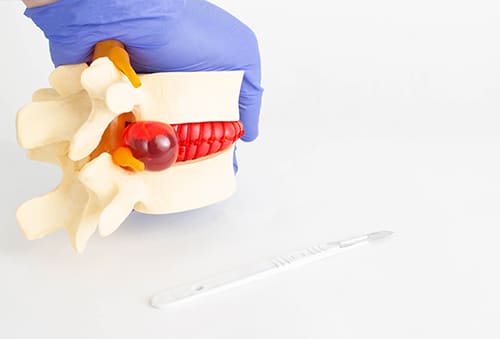
If a disc herniates or ruptures, the inner gel material leaks out of the discinto the spinal canal. Once the material makes contact with spinal structures such as nerves or muscle, it causes pain, irritation, and inflammation. The goal of a percutaneous discectomy is to eliminate pain by shrinking or removing the material surrounding the injured disc.
HOW IS THE PROCEDURE PERFORMED?
A percutaneous discectomy is minimally invasive.
The surgeon uses a medical imaging technique known as fluoroscopy to identify the problematic disc. Rather than making an incision in the skin, the surgeon uses fluoroscopic imaging to insert a needle into the disc. Using heat waves, the surgeon then removes the damaged disc material, easing pain and relieving pressure on compressed nerves.
A percutaneous discectomy can be performed using local anesthetic, which reduces the chance of complications.
WHAT SPINAL CONDITIONS CAN A PERCUTANEOUS DISCECTOMY HELP WITH?
A percutaneous discectomy can help manage pain associated with herniated discs and related nerve issues such as sciatica. Nerve pain can be debilitating and it can affect a patient’s quality of life – if your pain doesn’t cease after six months or so, then surgery might be considered.
There are various types of back surgery available; your specialist can advise if a percutaneous discectomy could help manage your condition.
WHEN IS A PERCUTANEOUS DISCECTOMY PERFORMED?
Non-surgical interventions are usually the first treatment of choice for disc herniations. However, a percutaneous discectomy may be performed if:
- You have a disc herniation
- Conservative treatments like painkillers and physical therapy have not worked
- You are in significant pain which affects your daily life
- There’s evidence of nerve impingement e.g. sciatica or radiculopathy
- The herniated disc material is pressing on a nerve root
It may not be the right treatment for patients with large, uncontained disc herniations in the spinal canal. It’s also not always appropriate for patients with stenosis.
To help identify if you’re a candidate for a percutaneous discectomy, your specialist may order imaging such as MRI scans to better visualize the herniation and identify the affected nerve roots. If you’re not a candidate, your specialist can discuss other treatments with you.
IS A PERCUTANEOUS DISCECTOMY SAFE?
A percutaneous discectomy is normally a safe, minimally-invasive, and effective surgical procedure. At the Interventional Spine & Surgery Group, we have performed many back surgeries including percutaneous discectomies, and we have helped thousands of patients find relief from back pain.
As with any surgical intervention, percutaneous discectomies do carry some risk. The risks are less than with open surgery; however, they include:
- Reaction to anesthetic
- Bleeding
- Nerve irritation
There’s also the chance the surgery will not be successful and you will still experience some pain and discomfort. Surgical results can never be 100% guaranteed.
HOW LONG DOES IT TAKE TO RECOVER FROM SURGERY?
As we can perform this procedure under local anesthetic, it’s much quicker to recover from a percutaneous discectomy when compared to other back surgeries. There’s minimal scarring and since there’s no damage to the bone or muscle tissue, recovery is less painful.
You will still be advised to avoid certain movements, such as excessive twisting or bending, for a few weeks following surgery. Every surgery is a little different – your specialist can discuss any specific rehab or post-op recovery instructions with you.
WHAT IF I DON’T WANT TO HAVE PERCUTANEOUS DISCECTOMY SURGERY?
Don’t worry – non-surgical treatments are often successful at treating the symptoms of a disc herniation, including sciatica. The treatments we offer at the Interventional Spine & Surgery Group include:
- Nerve blocks
- Physical therapy and exercise
- Medication
- Steroid injections
There are also other surgical treatments available, depending on your condition, medical history, and symptoms. The best way to find the right treatment for your needs is by contacting a spine specialist.
Contact our spine specialists now to book a consultation or discuss the percutaneous discectomy procedure in more detail.